Frank comes home after picking up a new prescription. At the pharmacy, he said he didn’t have any questions—but now he’s unsure how to take it. The label reads: “take two pills daily.” Does that mean one in the morning and one in the afternoon? Or both at the same time? Instead of calling the pharmacy or his doctor, Frank decides not to take the medication at all. He’s worried about getting it wrong.
Situations like this are more common than we think. Many patients face unclear directions, hesitate to ask questions, or avoid care altogether because they don’t fully understand their treatment plan.
On the South Central Telehealth Resource Center’s Telehealth Talk podcast, Allison Caballero, director for the University of Arkansas for Medical Sciences Center for Health Literacy, highlights the importance of using plain language when communicating with patients.
The Center for Health Literacy focuses on improving population health by making health information easier to understand and use. Clear communication about health information is essential for patient safety. The Joint Commission recognizes clear health communication as a key strategy for improving patient outcomes. In 2024, the Centers for Medicare and Medicaid Services (CMS) also introduced a new regulation requiring Medicare Advantage plans to identify and support patients with low digital health literacy.
How Health Literacy Supports the Quadruple Aim
Beyond regulatory requirements, health literacy supports the four Quadruple Aim goals: Patient Experience, Population Health, Reducing Cost, and Care Team Well-Being.
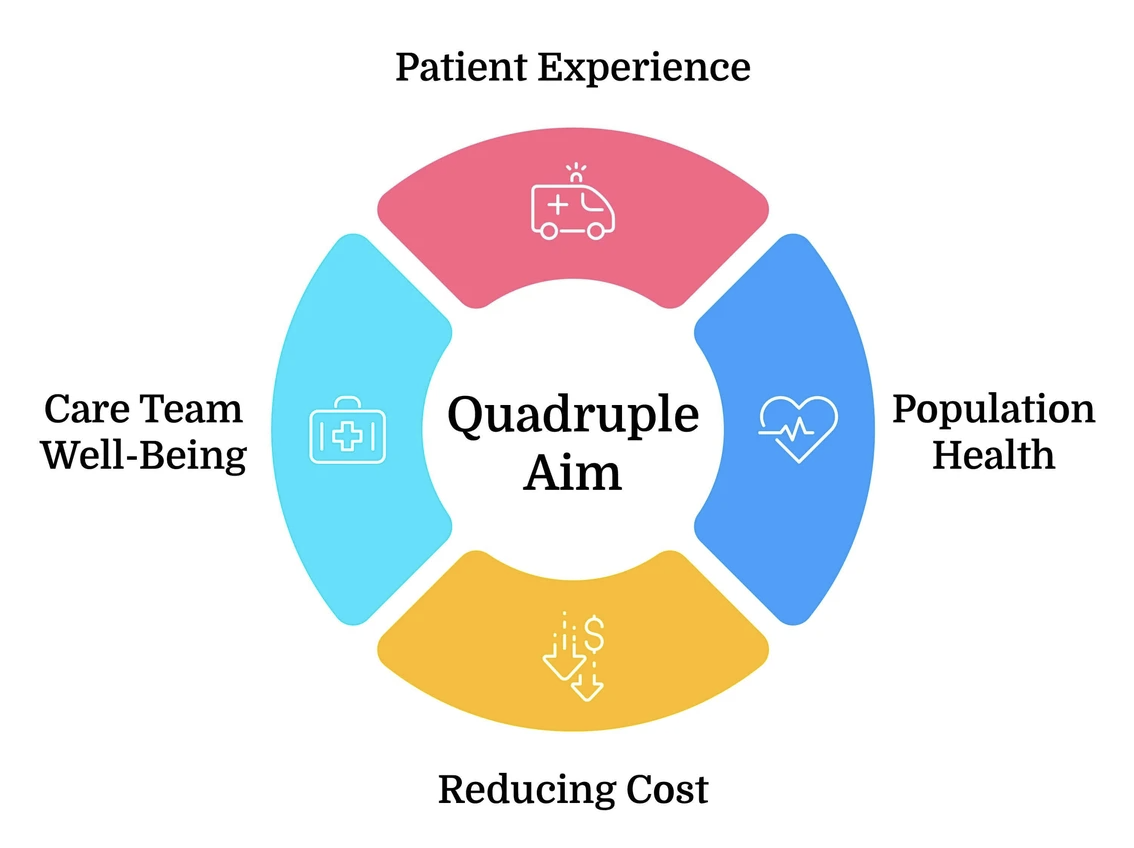
Patient Experience
When patients clearly understand their health information, they are more likely to follow care plans, take medications correctly, and engage in preventive care. This leads to better outcomes—and a better overall experience for both patients and providers.
Population Health
Clear, actionable information doesn’t just help individual patients. It can influence families and communities. When more patients understand how to manage their health, population-level outcomes improve over time.
Reducing Cost
Better understanding leads to better follow-through—like filling prescriptions, attending follow-ups, and completing preventive visits. These behaviors are often tied to value-based care metrics and can help reduce avoidable costs.
Care Team Well-Being
Providers want their patients to succeed. When communication is clear and patients are better equipped to manage their health, it reduces frustration and improves the care experience for the entire team.
Health Literacy Also Matters for Telehealth
Health literacy becomes even more critical in telehealth settings.
Digital care has expanded rapidly, but not all patients have the same level of access or comfort with technology. Some may be using telehealth for the first time, while others may lack reliable internet or depend solely on a smartphone.
In fact, about 9% of rural residents do not own a smartphone, and approximately 18–22% of low-income households lack reliable internet access.
This adds another layer to communication. Providers must not only explain health information clearly, but also discuss how to navigate the technology itself—logging in, enabling audio and video, and participating in a virtual visit.
Using plain language for both clinical and technical instructions helps patients fully engage in their care.
Why Does Health Communication Break Down?
Healthcare professionals spend years learning complex terminology—but most patients do not. Only about 12% of adults have proficient health literacy skills. This creates a gap between what providers say and what patients understand. When information is too complex, patients may struggle to interpret, remember, or act on it, leading to missed medications, skipped appointments, or poor health outcomes.
How Providers Can Improve Health Communication
Improving health literacy doesn’t require a complete system overhaul. Small, intentional changes can make a meaningful difference.
Start with plain language. This means using everyday words instead of medical jargon, explaining information the same way you would to a family member at the kitchen table.
Healthcare organizations can also look to the Agency for Healthcare Research and Quality (AHRQ), which outlines 10 attributes of health-literate healthcare organizations. Strong leadership and clear policies help ensure communication is consistent, accessible, and patient-centered.
Reviewing written materials is equally important. Instructions, discharge notes, and patient education resources should be easily understood the first time a patient reads them.
Teach Back Method
One of the most effective tools providers can use is the Teach Back method, which involves asking patients to repeat information in their own words to confirm understanding.
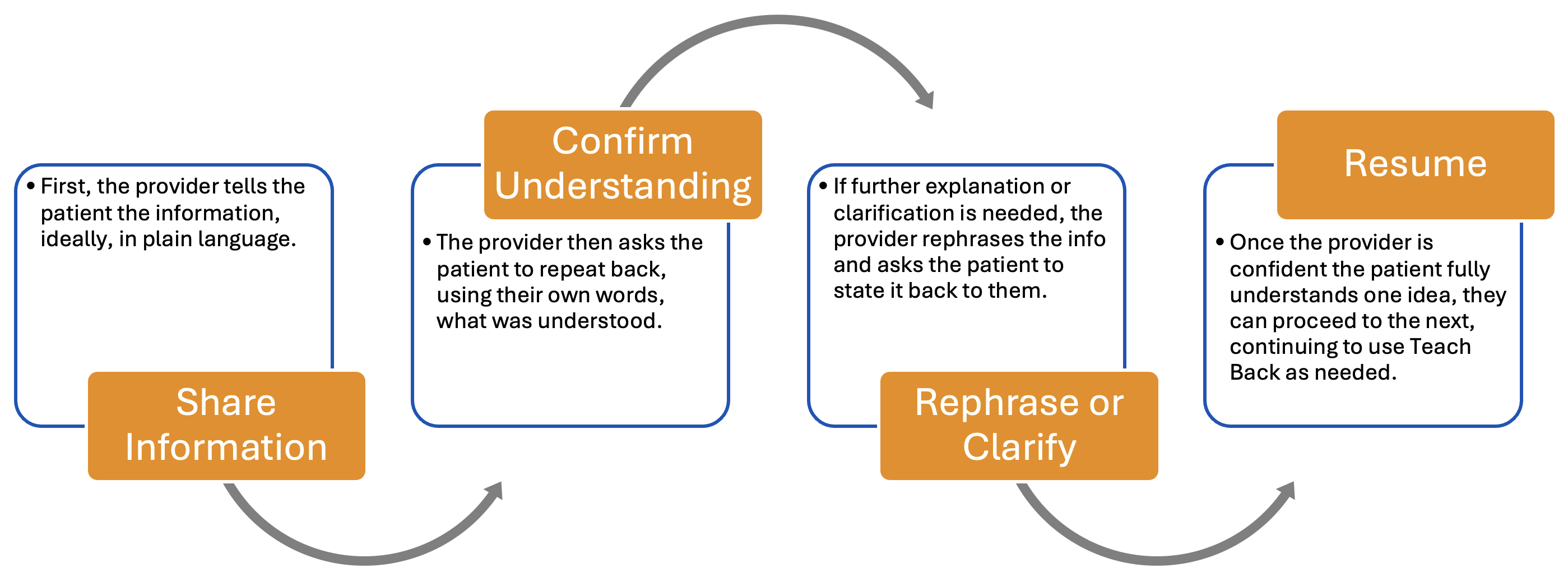
Final Thoughts
The key with health literacy is to start small, implementing step-by-step strategies that can make all the difference. Even if you can’t encourage your entire organization to implement new strategies, you are making a difference by choosing to practice plain language yourself. Continue to educate yourself and stay up to date on the best ways to ensure patients understand the health info you provide to them. It could be the difference between poor and improved health outcomes.


